Written by Marielle
Contents
The entire healthcare industry is financially linked to insurance providers who impose their own billing rules and requirements. Healthcare providers, including podiatry clinics, should comply with all these ever-changing regulations besides those set by the government, which makes medical coding and billing challenges.
Podiatry coding and billing are even more complex because the medical necessity of foot care and restrictions on foot conditions are specific. Podiatrists do not have the time to deal with all these intricacies, so they should outsource these tasks to a BPO company to receive optimal reimbursements.
Read on to learn about podiatry billing and coding and the factors affecting podiatry reimbursements. You will also learn about what a distinct procedural service is, why a podiatrist should outsource medical billing and coding, and how to identify an excellent external medical billing provider.
What Is Podiatry Billing?
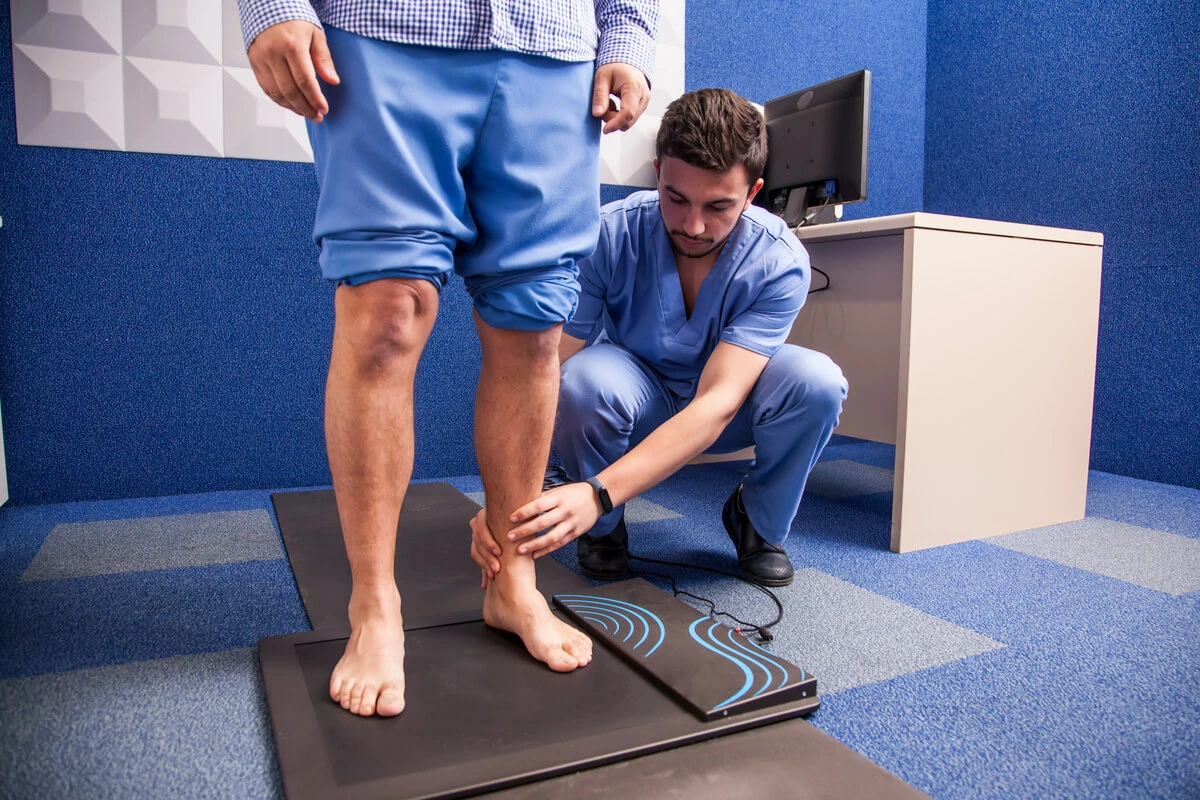
Foot problems, injuries, and abnormalities are the focus of podiatry. Podiatric medicine deals with the diagnosis, medicinal treatment, and surgical correction of foot, ankle, and lower-limb diseases. This expertise encompasses therapeutic, surgical, mechanical, and physical foot therapies.
Medicare does not cover the following services because it considers them routine:
- Cutting or removing corns and calluses
- Foot washing and soaks to maintain skin tone in ambulatory or bedfast patients, skin creams used to maintain skin tone, and any other treatment provided in the absence of localized sickness, injury, or symptoms affecting the foot
Podiatry billing and coding can be challenging in various ways, from establishing and verifying a treatment’s medical necessity to the subtleties of coding. Podiatry clinics also handle the elderly, which requires extra-billing and coding efforts because Medicare supports this demographic. Podiatry billing and coding require careful use of modifiers and knowledge of inclusive procedure coding.
Podiatrists can hire an in-house staff of coders or contract an experienced third-party billing service. A medical billing provider must be competent enough to systematically monitor, document, and remedy underpaid or unpaid claims.
With established best practices and seasoned personnel who can deliver accurate podiatry coding, collections can improve by 25%, and rejections can decrease by 23%.
What Are the Factors Affecting Podiatry Reimbursements?
Insurance providers can deny medical claims for podiatric services for several reasons. For example, a payer has stopped covering certain services or has already granted the maximum benefit for podiatric services in the claim.
The following are some factors in the successful and optimal reimbursements of podiatric services:
- Request for prior approval. Podiatry clinics often experience authorization rejections. They must obtain prior authorization from the insurance provider, adhering to its guidelines and specific formats. After receiving approval from the insurance provider, they can submit their claim and the authorization number.
- Medical necessity. Coders must be skilled in using diagnosis and Current Procedural Terminology (CPT) codes. They ensure that both the national coverage determinations (NCDs) and the local coverage determinations (LCDs) are applicable. Medical necessity is critical to the success of a medical claim. Coding documentation should reinforce the medical necessity of the services provided and billed by a podiatry practice.
- Accurate coding. Medical coding accuracy is critical to successful claim submission. The healthcare provider can individually bill additional procedure codes by the payer’s standards.
- Inclusive procedures. In most cases, an insurance provider denies a claim because the procedures are inclusive. A healthcare provider should not bill CPT codes 11719, 11721, and G0127 together to prevent inclusive rejections. If an insurance company denies a claim even with the necessary modifier, the biller can appeal and have the claim reviewed using the relevant medical documents and Correct Coding Initiative (CCI) amendments.
- Service recurrence. Once every 60 days, routine foot care is considered medically required. Because payers see frequent services as superfluous and inappropriate, they refuse them within 60 days. The biller can appeal with medical documentation proving the need for such a service.
What Are the Q Modifiers for Podiatry?
Insurance companies want to know why a doctor conducts foot care, and Modifiers Q7 (one Class A finding), Q8 (two Class B findings), and Q9 (one Class B and two Class C findings) can help them understand. Billers submit claims using Q modifiers that indicate findings related to a patient’s condition.
- Class A – non-traumatic amputation of the foot or an integral skeletal component
- Class B – absent dorsalis pedis pulse, absent posterior tibial pulse, and at least three advanced trophic changes (nail thickening, rubor or redness of the skin, absence or decrease of hair growth, skin discoloration, thin and shiny skin texture)
- Class C – temperature changes (e.g., cold feet), edema (swelling of a body part), claudication (pain in the arms or legs)
What Is a Distinct Procedural Service?
Modifier 59 (distinct procedural service) indicates that a procedure performed on the same day by the same practitioner is different from others billed on the same date of service. Mistakes could happen when coding multiple services not normally reported together.
Coders can use Modifier 59 in the following cases:
- A different session on the same date of service
- A different anatomical site or organ system
- A separate incision or excision
- A different lesion
- A separate injury
Why Should a Podiatrist Outsource Medical Billing Services?
Outsourcing can help boost patient care and employee productivity. A podiatrist’s job is to diagnose and treat patients experiencing problems with their feet and ankles. Podiatry billing and coding are a burden on podiatrists’ schedules every day.
External providers can better handle podiatry billing and coding because the medical necessity and restrictions on foot conditions are specific. Additionally, podiatrists should not waste their time understanding what services to cover under which insurance providers, using correct codes for different services, and submitting clean documentation.
Those tasks are necessary for optimal reimbursements. Professional billers and coders can do a better job at a fraction of the cost, and podiatrists can focus on treating their patients instead.
If a podiatry clinic outsources its medical billing and coding, it can have comprehensive performance reports submitted by the external team for transparency in operations. This is crucial for a podiatry practice’s success and sustainability. External medical billing companies can provide insights into billing operations.
How Do You Identify a Good External Medical Biller?
Podiatry billing and coding are challenging for several reasons.
Each insurance company has its own set of standards for determining whether surgery is medically required—and reimbursable—in a given situation. Because foot and ankle problems are increasingly common as people grow older, an aging population implies that Medicare will cover a growing number of patients, adding yet another set of codes and restrictions to the mix.
Outsourcing is becoming more common practice for medical offices and facilities. Individual medical billers working from home for medical billing organizations with thousands of customers are one possible option for outsourcing.
Medical billing is complex and requires a high level of competence and extensive experience when considering the various aspects of billing. A specialization like podiatry makes medical billing even more challenging to achieve success.
A medical billing firm must have a staff who understands the intricacies of the regulations followed by insurance companies to evaluate podiatry claims. In light of rising expenses, podiatrists must ensure that money is not being left on the table because their external billing provider is not an expert in the field.
Podiatry billing and coding businesses need to recognize the prevalence of at-home billers doing the tasks they claim to be experts in. Since remote employees are not operating in a supervised and regulated setting, situations like these carry a high level of danger.
The Bottom Line
Podiatrists are medical professionals who focus on diagnosing, treating, and preventing foot and ankle issues.
There are strict medical necessity standards and limits to foot conditions that podiatrists can treat. These healthcare professionals need to know what is covered, use the relevant codes for their services, and ensure that their paperwork is clean for optimal reimbursements. But they do not have to do these tasks if they outsource podiatry billing and coding to an external provider.
Podiatry billing and coding firms can manage all aspects of claims processing—including examining claims to ensure appropriate coding—validating benefits eligibility, sending out claims, and tracking all accounts receivable.
The documentation provided by professional coders and billers should be up to date according to the latest regulatory changes. To get the most out of an external podiatry billing agency, ensure it has a solid track record in the field and specializes in podiatry billing and coding.